Key Takeaways
- Bone grafting is essential for patients lacking sufficient jawbone structure for dental implants.
- Multiple grafting techniques exist, including autografts, allografts, xenografts, and alloplasts.
- Innovations like bioactive glass composites are revolutionizing bone regeneration.
- Risks exist, but they are manageable through careful planning and adherence to postoperative care.
- Consultation with a dental professional ensures personalized, successful implant outcomes.
Table of Contents
- Introduction to Bone Grafting
- Why Bone Grafting is Necessary
- Types of Bone Grafts
- The Bone Grafting Procedure
- Advancements in Bone Grafting
- Risks and Considerations
- Final Thoughts
Introduction to Bone Grafting
Bone grafting has become an indispensable part of dental implantology, offering solutions for patients with inadequate jawbone structure. This procedure involves supplementing or restoring bone in areas affected by resorption, disease, or trauma, creating a stable platform for future implants. In cities renowned for high-quality dental care, such as Miami, procedures like dental implants in Miami, FL often incorporate bone grafting to ensure optimal outcomes for patients.
Changes in jawbone anatomy can occur quickly following tooth loss, making timely intervention critical for anyone considering dental implants. Without adequate bone density, issues may arise, ranging from cosmetic concerns to limitations on the types of dental restorations that can be used.
Why Bone Grafting is Necessary
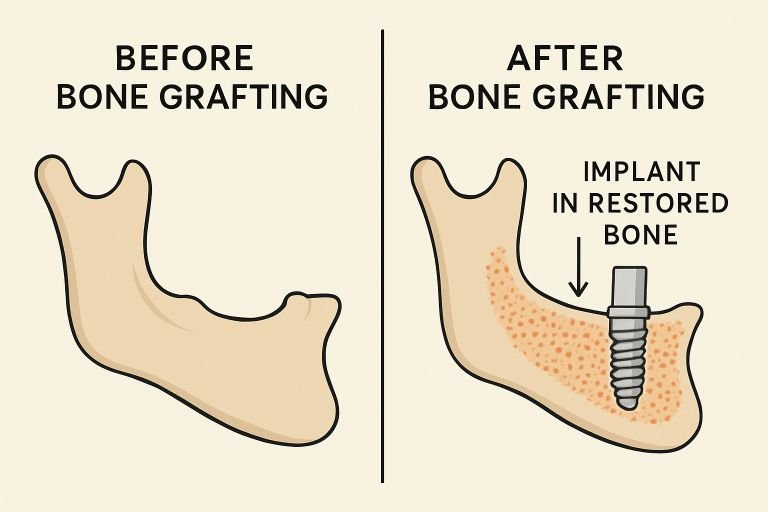
When a tooth is lost or extracted, the surrounding jawbone no longer receives mechanical stimulation from chewing, leading to bone shrinkage over time. This resorbed area may not support a dental implant, increasing the risk of implant instability or failure. Bone grafting replenishes lost volume and density, establishing the foundation necessary for a successful and durable implant.
Patients with a history of periodontal (gum) disease, facial injuries, or those who have worn dentures for many years are especially likely to require bone grafting before implant placement. This procedure restores both function and aesthetics, enabling patients to regain confidence and a restored smile.
Types of Bone Grafts
The choice of graft material depends on a variety of factors, including the patient’s oral health, the extent of bone loss, and personal preferences. There are four main categories of bone grafts used in current dental practice:
- Autografts: Bone tissue harvested from another site on the patient’s own body, such as the chin, jaw, or hip. This type eliminates the risk of rejection and is considered the “gold standard” for many procedures because it integrates quickly and reliably.
- Allografts: These grafts utilize bone from a human donor (usually cadaveric), which is thoroughly sterilized and processed for medical use. Allografts are a safe and effective alternative for those who are unable or unwilling to use their own bone.
- Xenografts: Derived from animal sources, most often bovine (cow) bone, xenografts provide a scaffold for the patient’s own bone cells to grow and remodel the area over time.
- Alloplasts: Synthetic grafts, typically made from biocompatible materials like medical-grade ceramics or bioactive glass, present a less invasive option with a low risk of disease transmission.
The Bone Grafting Procedure
The typical bone grafting process involves an initial assessment, during which the dental provider evaluates oral and bone health, often using advanced imaging techniques such as dental CT scans. Once a treatment plan is established, the area is numbed with local anesthesia, and the graft material is then carefully inserted at the deficient site. The surgical area is sealed—often using a special membrane—and allowed to heal. This integration process can take from several weeks to a few months, depending on individual healing factors.
During the healing process, the body works to remodel the graft, gradually building new bone tissue and replacing the graft material with the patient’s own cells. Upon successful integration, the area is ready for the placement of dental implants.
Advancements in Bone Grafting
Bone grafting technology is evolving rapidly. New biomaterials, such as bioactive glass composites, are being integrated into clinical practice, offering enhanced properties for bone regeneration. According to a recent study published on arXiv, bioactive glass can accelerate bone growth around the implant site, improve the quality of bone-to-implant contact, and reduce healing times.
Risks and Considerations
As with any surgical procedure, bone grafting comes with potential risks. The most common complications include infection at the graft site, rejection of graft material, and surgical side effects such as swelling or discomfort. Less commonly, patients may experience numbness if nerves are disturbed during surgery. Adhering closely to post-operative care instructions—such as prescribed medications and oral hygiene practices—can greatly minimize these risks. Discuss all potential risks and your medical history thoroughly with your dental specialist before undergoing a grafting procedure.
Final Thoughts
Bone grafting is a foundational step for many successful dental implant treatments. By restoring lost jawbone, the procedure not only makes dental implants possible but also supports long-term oral health, stability, and confidence. Thanks to modern advancements, dental professionals can offer effective, individualized solutions for a wide range of patients. Consider consulting a dental implant specialist to explore your options and ensure the best outcomes for your oral health journey.