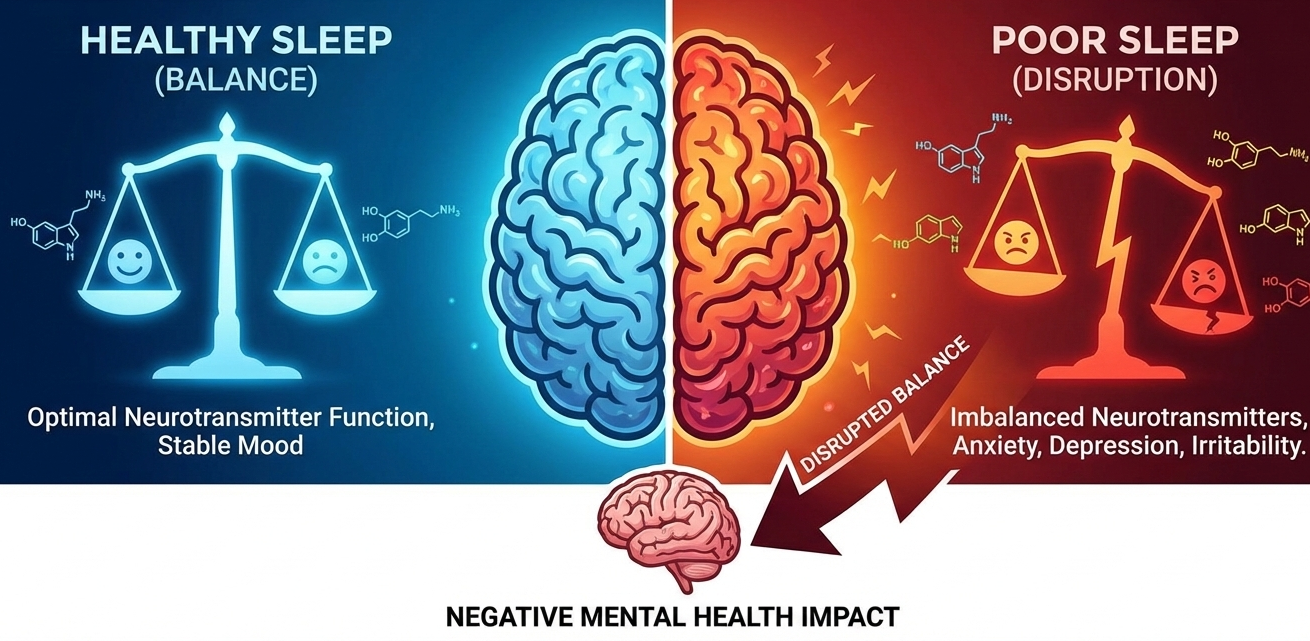
Global health crises of recent years such as the COVID-19 outbreak or Ebola outbreaks have brought out one conspicuous truth: although personal protective equipment (PPE) protects the body of the health worker, they do very little to protect their mind. Personal protective machinery, such as masks, gloves, and clothing is necessary, as well as the psychological equipment of health workers that lets them resist the psychological and emotional pressure of high-stress conditions.
Mental burnout, moral injury, and post-traumatic stress disorder (PTSD) are starting to overwhelm frontline health workers. Amidst these increasing demands there is a lack of development of mental resilience in health workforce training and a lack of focus on it.
The purpose of my article is to bring into the limelight the other side of the attribute; that is psychological resilience. It involves a paradigm change in the health systems-a change that embeds resilience training, stress management and mechanism of coping into the design of a health system including healthcare education and deployment.
Learn more about why the proactive mental health education issues is instrumental and why it is a sustainable healthcare practice.
The PPE Paradox: Physical Protection Without Mental Défense
As the result of pandemics and crises, the world has appropriately been concentrating on the stock of PPE. There is much truth to this saying that under the context of protecting bodies, many systems have not emphasized their efforts on what is beneath it all: the emotional fatigue of workers who are up with death, trauma, and doubt all the time.
The Paradox is Simple: we must keep the outside safe, but reject the inside.
- A mask hides airborne infections but can’t filter despair.
- A face protects blocks fluid, but do not shield anxiety.
- Gloves stop your hands from being exposed to infection, not emotional burnout.
Health workers walk around with invisible scars because they lack psychological armor and these injuries get compounded with time-eventually affecting their well-being, judgements and ultimately the patient care.
Why Psychological Resilience Matters in Healthcare
The psychological resilience does not mean the one is capable of surviving. It is the conditioned ability to bounce back, change and become stronger even when there is trouble. Resilience can have a direct impact on the sustainability of health workers, who may sink into burnout or even collapse early, or have a long-term professional life.
- Combating Burnout
The rates of health professional burnout in the world have never been higher. The powerful army will not be affected by:
- Emotional distress
- Depersonalisation that is becoming cynical or indifferent
- Low personal accomplishment
- Improving Patient Care
Health workers with effective coping abilities produce better decisions, message more precisely, and have lots of empathy, which will have an immediate patient outcome.
- Enhancing Workforce Retention
Attrition will be minimized by psychological care. When employees feel psychologically or morally stable, there is a greater likelihood of them retaining their jobs, particularly in environments that expose an individual to serious health risks like emergency departments or areas of disease outbreaks.
The Science Behind Mental Resilience
Resilience is not an inborn good fortune: it is a skill a person may be taught, trained and developed. According to neuroscience and psychology studies, there are essential elements of resilience training which are as follows:
- Emotional Regulation: Finding the way out of processing fear, grief, anger, and not being overwhelmed by them
- Cognitive Reframing: Changing the view stressors are seen
- Mindfulness and Self awareness: Control increase over a person state of mentality
- Social Connection: Establishing reliable helping system
- Meaning Making: Purpose in their role to help develop motivation and mitigate feeling of despair
Such practices could be built into health education and job culture that creates a new generation of medical professionals: not only educated clinically, but with the armor in their minds.
What Does “Beyond PPE” Really Look Like?
What is required is more than PPE, and that is to incorporate psychological safety into the genetic code of healthcare systems. It is about the concept of mental health awareness being lent to action with systematic programmes, instruments and institutional dedication.
- Integrating Mental Resilience into Health Curricula
Medical and nursing schools usually teach much more about diagnostics and procedures and not much about psychological preparedness. All health workers, no matter where they work, are going to experience death and suffering and pressure of the system.
Proposed Approach:
- It is a good idea to integrate resilience training courses into any course in healthcare
- Introduce into education, at an early age, the reflective practice and the group processing
- Run case studies to be able on talking about moral coping responses and dilemmas
- Educate learners in stress prevention techniques such as; breathing exercises and mindfulness.
Such proactive mental health education at the foundational level can create a workforce that is more capable of dealing with any crisis that lies ahead.
- Resilience Workshops for In-Service Professionals
Mental resilience is something that one can be shaped into even after they are practicing. Measures to be administered by hospitals and health ministries should include:
- Annually or quarter resilience establishing workshops
- First aid training for mental health
- Programmes of peer-to-peer mentorship, the latter doing a psychological support.
The emotion work is also normalized in interactive scenario-based training that would provide SH with the space to think about this experience.
- Institutional Mental Health Support
In the same way that hospitals offer labs and pharmacy, it is in their capacity to extend to offering mental health infrastructure. This may include:
- Virtual or being on site access to professional psychologists and counsellors
- Anonymous mental health crisis helplines are to help in case of emotional crisis in case of an emergency.
- The generic employee appraisals are mental health screening instruments
- Policies for mental health leave, to be able to recover and prevent burnout
Strengthening culture through the means of making sure that support services are visible, accessible and non-stigmatized helps support the idea of help-seeking behaviour.
- Workplace Culture That Values Emotional Wellness
Leadership is a way of having a resilient system. Emotional wellness should not be viewed as optional; all administrators need to create a culture where it is regarded as a necessity.
This includes:
- Regular checking by supervisors not only performance wise, but also emotion wise
- Lighting up the so-called free discussion of the degree of stress, trauma, and mental load
- Bolding emotional resilience in performance evaluations and metrics
The creation of psychologically secure working environment will enhance spirits and productivity.
Case Studies: What’s Working Around the World?
Canada – “The Resilience Project”
Structured group debriefings following critical incidents, mindfulness sessions and hospital employees getting access to licensed therapists have all become part of the practice of health facilities across Canada.
Results:
- Reduction of about 40% in stress related absenteeism
- An increase in high level job satisfaction among emergency departmental staff
India – “Mental Wellness Circles”
Some hospitals have introduced internal wellness circles, peer-led support groups, in which the staff meetings once a week to share their feelings, challenges, and strategies to cope in the time of COVID-19.
Outcomes:
- Better team cooperation
- Reduction in turnover during high level crisis period outbreaks
Kenya – “CHEW Resilience Integration”
The monthly meetings arranged by Community Health Extension Workers in high-risk areas involve resilience training to the CHWs.
Impact:
- Strong community trust
- Better follow-up care since they reported more of strains on emotions
Breaking the Stigma Around Mental Health in Healthcare
The first is the impact of stigma regarding mental health as a significant impediment in actualizing psychological resilience training. The issue that intimidates most professionals in health is a perception that they will be weak by admitting they had problems.
To overcome this:
- Use strong formal languages such as “resilience making” instead of “therapy”
- Have well known professional educated health leaders share personal details of their emotional issues.
- Incorporate mental health into the current health education by way of not an extracurricular topic, but an ordinary part
Such transition is possible with the help of recontextualizing of mental health as a feature of professionalism rather than vulnerability.
The Cost of Ignoring Psychological Protection
It is costly to do nothing. The non-satisfaction of mental health will result in:
- Medical errors increase
- Labour attrition in already stressed systems
- High cost of sickness and low rate of productivity
- The impairment of care through a condition known as compassion fatigue
- Low confidence among the people in the crunched and emotionally distant providers
The concept of mental resilience is not a luxury anymore. It is necessary in the current society to deliver sustainable healthcare.
A Call to Action: Building Resilient Health Systems
- The management, position of organizations, and educative powers must make sure that the psychological protection becomes obligatory like physical PPE. This includes:
- Investing money for mental resilience programs
- Attending to resilience indicators of healthcare quality measurement
- Cooperating with mental health institutions in developing contextualised curricula
Implementation of the mental health protection in labour policies and documents concerning staff rights
Conclusion: Equipping the Mind as Well as the Body
Medicine is a human activity. Despite all the skills and as immediate background that they are, human beings are not under the exception of emotional fatigue. PPE provision of health workers is non-negotiable anymore.
We should take it another step further and equip them with the psychological knowledge to maintain their enthusiasm, guard their mental safety and emerge above the challenge. It is with structured, culturally sensitive and proactive mental health education that we develop efficient, but also humane health systems.
Since, with health workers whose well being is intact, the well being of services they provide is intact.